Imagine: suddenly, you can no longer smell your favourite perfume or dish. Many COVID-19 patients know all about it: they lost their sense of smell and taste. But, does losing these senses prompt different eating behaviour? And: can you recover your sense of smell? There is hope for these patients, says Elbrich Postma, set to graduate for her PhD on 15 January at Wageningen University & Research. Her research focuses on the effect loss of taste and smell has on eating behaviour and brain activity.
Losing one's sense of smell impacts quality of life, says Elbrich Postma. 'Patients do not enjoy their food as much and are at risk because they can no longer smell smoke or gas. Moreover, they may become self-conscious about their body-odour or even experience depression.'
Patients who lose their sense of taste and smell are confronted with this fact every day, at every meal and with every snack. Between 5 and 20 per cent of the Dutch population suffers from a diminished sense of taste or smell. There are many different causes, such as the common cold, flu, an accident or ageing.
To date, little is known about the effects of a diminished sense of taste or smell on eating behaviour and the impact on the areas in the brain responsible for detecting smell or taste. Elbrich Postma, of the Human Nutrition & Health group, studied whether patients do, indeed, adopt a different eating pattern from people whose sense of smell and taste are intact. Contrary to her expectations, she discovered that patients are as likely to eat according to the Dutch Dietary Guidelines as the average Dutchman.
Food intake is determined by various factors, such as the social situation and learned eating habits, and not just by smell or taste. However, patients born without a sense of smell who have been unable to smell from birth, favour foods with a stronger taste component to compensate for the loss.
Loss of smell and brain activity
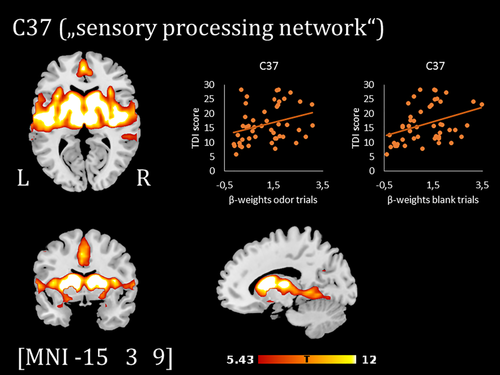
Postma also studied the effect of reduced smell on the brain. To this end, she had patients smell certain odors while subjected to an MRI scan. This research was conducted in the MRI facility of the Gelderse Vallei Hospital. 'Initially, patients doubted the usefulness of this exercise', Postma states. 'After all, they smelled nothing, so how would they suddenly experience odors in the MRI?' Although the patients indicated they smelled nothing, their brains showed a response to the different scents. 'The sense of smell was still basically present. This offers opportunities for the treatment of patients who have recently lost their sense of smell', says Postma.
Scent-training to regain sense of smell
'Possibilities include smell training, similar to how one would offer physiotherapy. We ask patients who are confronted with the odor of, for example, roses, to focus on their previous experience with that fragrance. Through practice, you may be able to restore the link with the brain, and thus regain the experience of the scent of roses.'
The Wageningen researcher also found a link between the so-called orbitofrontal cortex - the part of the brain located almost against the forehead that is involved in the integration of taste and smell- and how well patients can smell. This shows that it is vital for future research to link changes in eating behaviour and changes in the brain. Therapies such as smell training may have a limited effect on the sense of smell, but they may still lead to changes in the brain,' Postma concludes.
Dissertation
Coming to your senses: Effects of changes in olfactory and gustatory function on eating behaviour and the brain - PhD defence Elbrich Postma, Wageningen University & Research, 15 January 2021.






