Connie Way came from the Midwest to San Francisco in the late 1960s, landing a job as a telephone operator for Pacific Bell. There, she met her husband, Bill, and together they raised two sons. Her life was full and exciting, and when retirement came it read almost like a storybook. The couple moved to Stonyford, at the edge of the Mendocino National Forest, embracing a slower pace of life.
 Connie Way is fighting esophageal cancer with the support of her son Eric Way and UC Davis oncology surgeons.
Connie Way is fighting esophageal cancer with the support of her son Eric Way and UC Davis oncology surgeons.
Then came health challenges. First, Bill passed away from lung disease in 2015. Now, Connie is fighting with everything she has to battle stage III esophageal cancer. As April is Esophageal Cancer Awareness Month, she wanted to share her story to help others.
"I never thought that I would get cancer," said Way, now 74, who was diagnosed in the middle of the COVID-19 pandemic. "Giving up wasn't an option, though, and I am grateful that recent advancements in fighting esophageal cancer have worked in my favor."
Way's oncologist at Adventist Health + Rideout Cancer Center started her on chemotherapy and radiation, and her tumor shrank to nearly 3 centimeters. Her oncologist felt that because Way's case was complicated, the next best step was surgical treatment at the UC Davis Comprehensive Cancer Center, where advances in video-assisted robotic technology could provide the best outcome.
Symptoms and prevention of esophageal cancer
Esophageal cancer is three to four times more common among men than women, and the risk of the disease increases with age. Most esophageal cancers are squamous cell (risk factors include tobacco and alcohol use) or adenocarcinomas (often caused by acid reflux and being overweight). Although the incidence of squamous cell carcinoma is decreasing in the United States, the incidence of reflux-induced adenocarcinoma is dramatically rising.
Early esophageal cancer may not cause symptoms. As the cancer grows, the most common symptoms are:
• Pain when swallowing or food getting stuck
• Pain in the chest or back
• Weight loss
• Heartburn
• A hoarse voice or cough that doesn't go away within two weeks
People who suffer from persistent reflux symptoms should talk to their doctor about the risk of esophageal cancer. Over time, the acid that backs up into the esophagus can damage the lining and lead to a condition called Barrett's esophagus. People with Barrett's esophagus are at a much higher risk of developing esophageal cancer.
UC Davis Health opened a unique clinic in 2019 that provides an all-in-one treatment program to control gastroesophageal reflux disease or GERD.
"We wanted an interdisciplinary team approach to taking care of patients with reflux with the ultimate goals of improving quality of life and preventing esophageal cancer," said Peter Belafsky, co-director of the UC Davis Reflux Clinic. "In the two years we've been open, the patient load has increased dramatically—especially since the onset of COVID-19 when the stress caused by the pandemic has created an alarming demand for GERD treatment."
That's where Way met Lisa Brown, assistant professor of general thoracic surgery at UC Davis and a national expert on minimally invasive surgery for complex esophageal disease, and David Tom Cooke, chief of general thoracic surgery, director of the UC Davis robotic thoracic surgery program and a national expert on the surgical treatment of esophageal cancer. Together, the surgeons teamed up with the robotic da Vinci Surgical System to perform the intricate surgery and successfully remove the tumor.
"I'm still walking, talking and breathing and I feel so fortunate to have been seen at the UC Davis Comprehensive Cancer Center," said Way.
UC Davis performs the highest volume of robotic thoracic surgery in the region. Robotic Esophagectomy, as it is called, results in less pain and faster return to activities of daily living.
"We are proud to offer complex and innovative resources such as robotic surgery to support our patients as we push the envelope to restore the health of our California communities," said Cooke.
Novel alternatives to surgery
Not all patients with esophageal cancer are treated with surgery. UC Davis oncologists use novel immunotherapy drugs known as checkpoint inhibitors to treat the cancer.
And, there are new non-surgical solutions that UC Davis gastroenterologists like Shiro Urayama use such as radiofrequency ablation, photodynamic therapy and cryotherapy to treat pre-cancerous conditions of the esophagus.
Urayama is renowned for performing advanced endoscopy interventions including endoscopic submucosal dissection (ESD), which uses an electrocautery knife to burn and carve out large, flat lesions from the esophagus. Patients often go home the same day. Thanks to Urayama's quest to be trained in the latest endoscopic weapons to fight esophageal cancer, UC Davis performs more ESDs than anywhere in California.
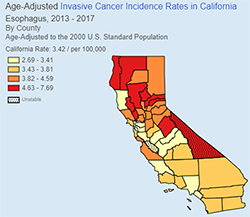
"The reason we need to be cutting edge at UC Davis is because of the volume of esophageal cancer patients we see who need these lifesaving procedures," said Urayama. "The rate of esophageal cancer is higher than average in our region, especially in the northern portion of the Central Valley."
It's not known why there is a higher rate of esophageal cancer in our region. More research needs to be done. What's essential is that anyone with ongoing symptoms of acid reflux or swallowing difficulty should be carefully evaluated with endoscopy and routinely monitored if indicated.