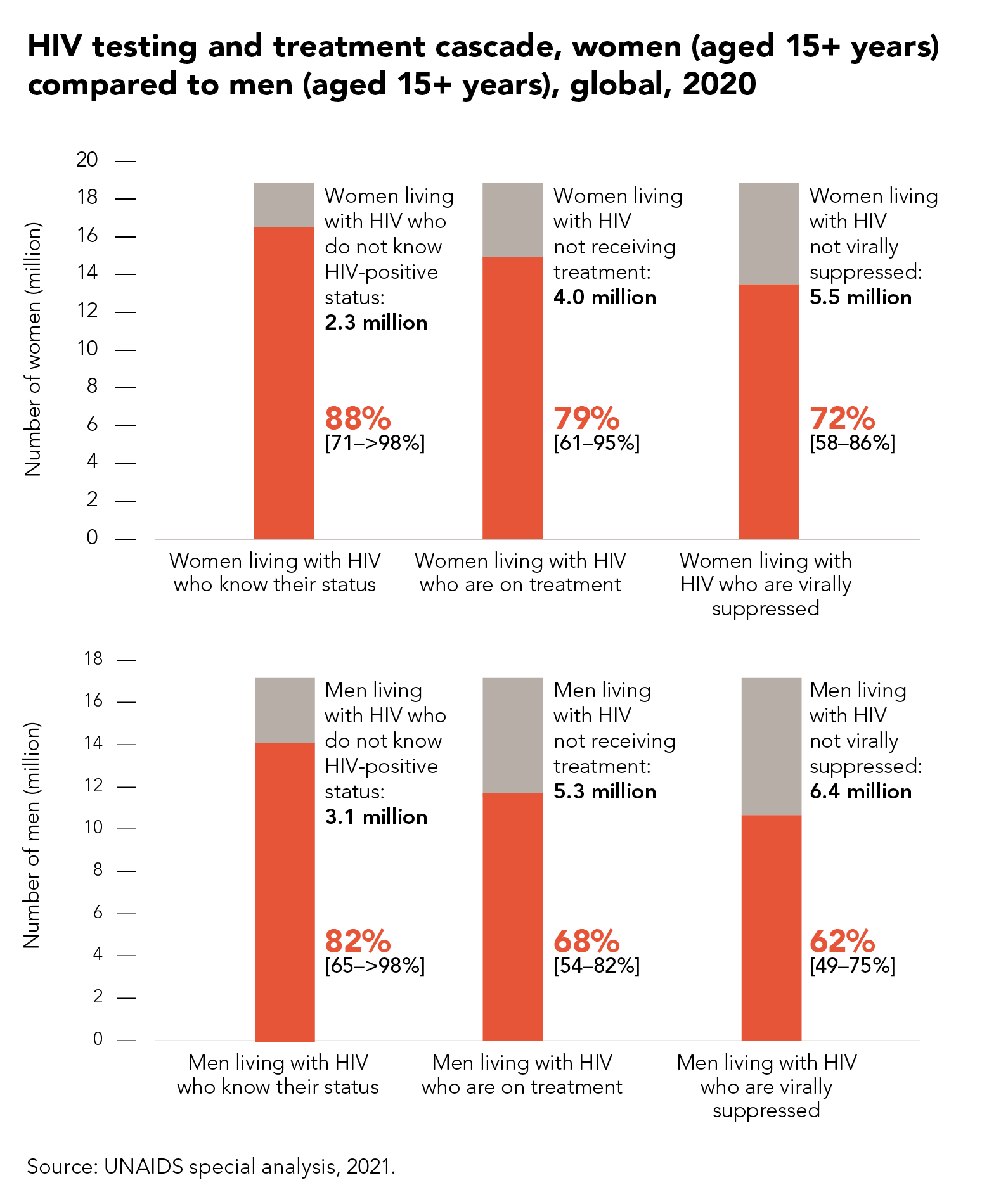
Globally, the testing and treatment targets for 2020 were almost reached among adult women (15 years and older) living with HIV. Men living with HIV, however, are consistently faring worse than women across the HIV testing and treatment continuum. Compared to women living with HIV, there are 740 000 more men living with HIV who do not know their HIV status, 1.3 million more men who are not on treatment and 920 000 more men who are not virally suppressed.
While gender norms that prize male strength and stoicism may partly explain why many men delay seeking care, other factors are also at play. Primary health-care services in eastern and southern Africa place a great deal of focus on women of reproductive age, and reproductive, maternal and child health services offer ideal entry points for HIV services; similar entry points for men are not commonplace. Interventions to reach and include men more successfully in HIV testing and treatment services are increasing-including through workplace-based interventions and greater use of self-testing approaches, and by providing services at outpatient departments-but a more finely-tuned understanding of why men's use of HIV services continues to lag can help shape additional ways to close this gap.