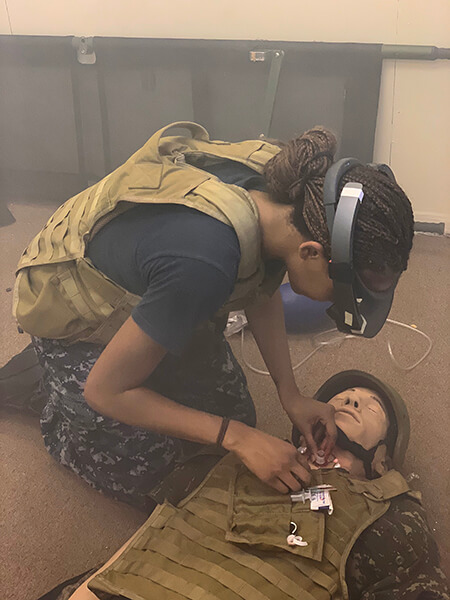
 In a smoke-filled room, a first responder receives instructions from a surgeon through an augmented reality headset to perform an operation. (Purdue University photo/Edgar Rojas Muñoz)
In a smoke-filled room, a first responder receives instructions from a surgeon through an augmented reality headset to perform an operation. (Purdue University photo/Edgar Rojas Muñoz) WEST LAFAYETTE, Ind. — War zones can be too far from operating rooms, preventing soldiers from receiving the surgery they need fast enough.
A Purdue University-led study is the first to show medics successfully performing surgery in life-like simulations of these war zones by receiving guidance from surgeons through an augmented reality headset.
The headset transmits a recorded view of the operating site to the surgeon, who can then use a large-display touch screen to mark up the recording with drawings of how to complete the surgical procedure. Augmented reality helps the first responder see the surgeon's annotated instructions directly on their view of the operating field.
Researchers at Purdue and the Indiana University School of Medicine have been developing this technology, called System for Telementoring with Augmented Reality (STAR), since 2015.
Operating rooms across the U.S. have already started using augmented reality telementoring to virtually bring in the expertise of other surgeons on how to use a new instrument or better perform a particular procedure.
But this technology hasn't made it to "austere" settings, such as a battlefield or forest thousands of miles away from a hospital, where a first responder could be treating injuries far too complex for their level of expertise, said Juan Wachs, Purdue University's James A. and Sharon M. Tompkins Rising Star Associate Professor of Industrial Engineering.
"Augmented reality telementoring doesn't usually operate well in extreme scenarios. Too much smoke can prevent visual sensors from working, for example," Wachs said.
Researchers from Purdue and the IU School of Medicine tested STAR with first responders and surgeons at the Naval Medical Center Portsmouth in Virginia. The work is published in NPJ Digital Medicine, a Nature Research Journal.
The study evaluated first responders using STAR to perform on a patient simulator a common procedure that opens up a blocked airway, called a cricothyroidotomy. Even the responders with no or little experience performing this procedure prior to the study successfully operated after receiving instructions from surgeons through STAR.
The simulations took place both indoors and outdoors, including smoke and sounds of gunshots, explosions and helicopters. The researchers found that first responders more successfully performed the cricothyroidotomies with STAR than with just hearing a surgeon's voice for each of these scenarios. If smoke made the visualization too unreliable, the responders could still do the operation when STAR automatically switched to audio-only telementoring.
STAR would need more durable materials before it's used on a real battlefield, Wachs said, but the software is now proven to work in extreme conditions.
Wachs has recently formed a company, AI-Medic, that is working on artificial intelligence solutions to address communication disruptions that might occur while using augmented reality telementoring systems in the field.
STAR is protected by patents filed through the Purdue Research Foundation Office of Technology Commercialization. This study was financially supported by Office of the Assistant Secretary of Defense for Health Affairs (Award No. W81XWH-14-1-0042) and the National Science Foundation (Grant DGE-1333468).






