Diabetes cost the UK almost £14 billion in 2021/22, including more than £10 billion in direct costs to the NHS, according to the findings of a new study which looked at the direct and indirect costs of the disease.
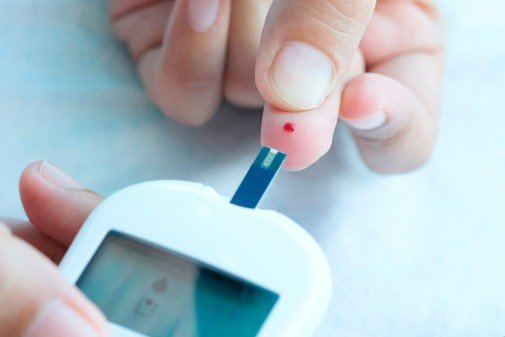 Complications from diabetes continue to account for the largest proportion of disease costs.
Complications from diabetes continue to account for the largest proportion of disease costs.
Despite the introduction of new technologies to tackle diabetes, researchers say it accounts for 6% of the UK health budget.
The study, which looked at the direct and indirect costs of type 1 and type 2 diabetes, and gestational diabetes, showed that just over 40% of costs were related to diagnosis and treatment, with the rest, at just over £6 billion, relating to excess costs of largely preventable complications.
Researchers warn that continued investment is needed in order to mitigate future costs, particularly as cases of type 2 diabetes continues to rise in younger people.
Diabetes complications
Researchers at York Health Economics Consortium conducted a similar analysis in 2012 and this latest report, although not directly comparable with the earlier study due to the use of different data sources, showed that the proportion of costs relating to diabetes complications has reduced over time.
Despite this reduction, however, complications from diabetes, such as stroke, amputation, and angina, still continue to account for the largest proportion of disease costs. Indirect costs, the productivity loss from absence from work or death, is estimated at £3.3 billion annually.
Nick Hex, Associate Director for the NHS and Public Sector at the York Health Economics Consortium, University of York, said: "Diabetes is a debilitating disease that affects people on a daily basis on many different levels. It remains a considerable cost burden to the NHS, and the majority of those costs are still spent on potentially preventable complications.
"Increased investment in new technologies that help people manage their condition contribute to some of the high ongoing costs, but the rise in type 2 diabetes in under 40 year-olds is a particular concern and there needs to be continued focus on prevention strategies."
Data gap
The study also revealed gaps in data collection on diabetes, which need to be addressed to ensure continued improvement in the quality of care for people with diabetes.
Nick Hex said: "It is really important that we have access to data that looks at the resources used on the disease by sex, ethnicity, and location so that we can get a better understanding of some of the drivers behind clinical decisions, and where there is greatest need for financial investment.
"It is also essential that health commissioners continue to invest in diabetes prevention, care and treatment to reduce future cost implications."
Early care
There are estimated to be more than 5.6 million people living in the UK with diabetes. With the right treatment and support, it is possible to live well with the condition. But without it, serious complications can develop and every week, diabetes leads to 2,990 cases of heart failure, more than 930 strokes and 660 heart attacks, and 184 amputations.
The research is supported by Diabetes UK, and they say the findings not only highlight the seriousness of diabetes, but also the huge opportunity to transform lives through a greater focus on early care and support, with fewer people developing complications.
Reduce harm
Colette Marshall, Chief Executive at Diabetes UK, said: "This new research paints a stark picture, with billions of pounds being spent treating devastating diabetes complications. These complications cause untold hardship to many thousands of people and are, in most cases, preventable with the right care.
"Shifting the dial from crisis to preventative care would help to reduce the harm from diabetes, allowing people with the condition to live well while, ultimately, reducing the cost to the health service."