It's a modern scientific renaissance: Little more than half a century ago, psychedelics were largely outlawed, squelching emerging research into the mind-opening substances. Today, psychedelics have moved from pariahs to potential treatments showing encouraging clinical trial results.
Here are four ways UC San Francisco researchers are pioneering new treatment frontiers in depression, Parkinson's, and addiction, thanks in large part to federal science funding support.
Rewire the brain to help beat depression
Psilocybin is the compound behind "magic" mushrooms' psychedelic powers. Used for millennia in traditional medicine, psilocybin also affects serotonin, a chemical our bodies produce to help regulate mood and emotions.
UCSF Ralph Metzner Distinguished Professor in Neurology and Psychiatry Robin Carhart-Harris , PhD, is among the world's first researchers in the modern era to demonstrate psilocybin's promise for treating depression. Carhart-Harris also directs the Neuroscape Psychedelics Division at UCSF .
What he found
In 2022, Carhart-Harris compared brain scans of clinical trial participants with depression before and after taking psilocybin under carefully monitored conditions. The scans showed significant changes in how different parts of the brain communicated.
Simply, psilocybin appeared to loosen the rigid brain patterns associated with depressive thinking , potentially helping patients break free from cycles of negative, repetitive thoughts. No such changes were seen in trial participants who had been given one of the most commonly prescribed antidepressants, escitalopram, suggesting that psilocybin acts differently on the brain than traditional treatments.
Why it matters
About 1 in 10 Americans report a recent bout of depression. Still, antidepressants are far from perfect and may not work for everyone. Carhart-Harris's work confirms that psilocybin could, one day, be a real alternative to traditional depression medications, including for people living with treatment-resistant disease.
Depression
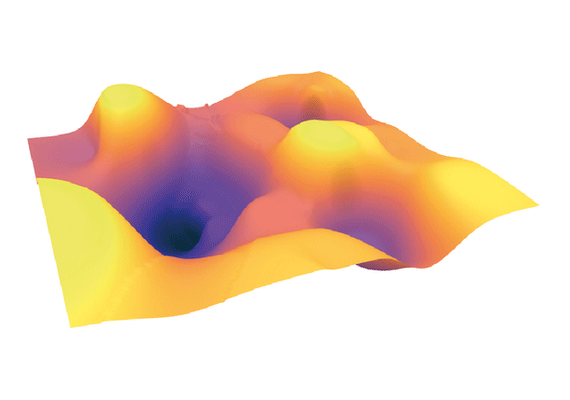
Psilocybin

Post-treatment

Images by Richard Daws, Kings College London
Ease Parkinson's symptoms
Assistant Professor Ellen Bradley , MD, runs a clinic focused on the neuropsychiatry of Parkinson's disease at the San Francisco Veterans Affairs Medical Center. Bradley and Associate Psychiatry Professor Joshua Woolley , MD, PhD, conducted the world's first study on psilocybin's effects on a neurodegenerative condition, in this case, Parkinson's disease. In addition to movement problems like tremors and stiffness, many people with Parkinson's also experience depression, anxiety, and other hard-to-treat mood problems.
What they found
The study, led by Bradley, showed psilocybin was safe and did not worsen Parkinson's symptoms, but, just as importantly, led to meaningful and sustained improvements in anxiety and depression as soon as one week after receiving the drug. Patients also reported better motor function following treatment. Although researchers aren't sure why, it may be that psilocybin directly affects brain systems involved in movement, or simply that feeling better mentally helps people move better.
Why it matters
Parkinson's disease is the second most common neurodegenerative disorder in America and affects about 1 million people in the U.S. Mood symptoms like anxiety and depression often precede the onset of the disease's more characteristic movement problems and are linked to a faster physical and cognitive decline. The results, Woolley says, raise the "exciting possibility that psilocybin may help the brain repair itself." A larger, follow-up study is underway.
Treat depression and anxiety - without the trip
LSD, short for lysergic acid diethylamide, is a powerful psychedelic best known for causing vivid hallucinations and dramatic shifts in mood, perception, and sense of time. Like psilocybin, it works by activating serotonin receptors in the brain. But because LSD's effects are longer-lasting and often more intense, it has been more challenging to study as a potential depression treatment.
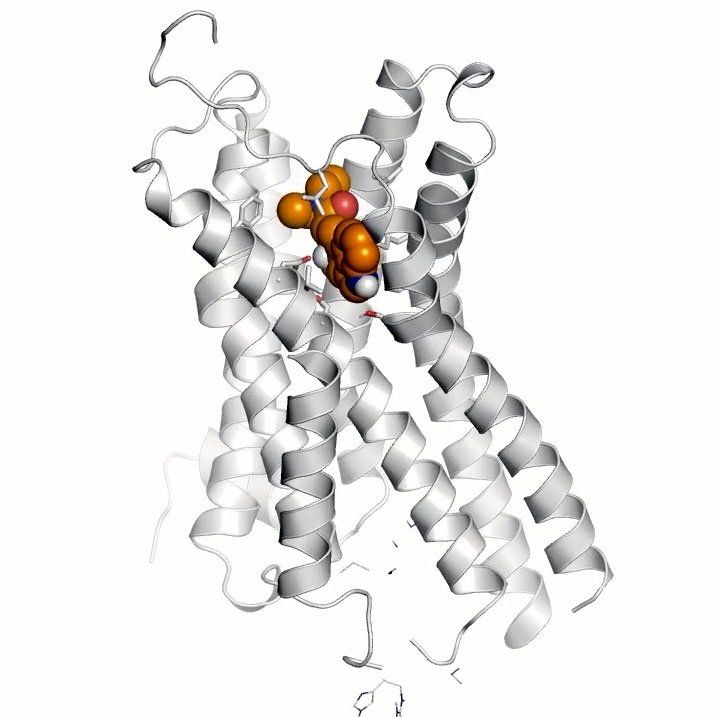
What they found
Pharmaceutical Chemistry Professor Brian Shoichet , PhD, and his team collaborated with groups at Yale, the University of North Carolina at Chapel Hill and Duke University to screen virtual chemical libraries to discover new molecules that target the same key receptor that LSD activates - without triggering hallucinations. In early laboratory studies, a single dose produced durable, antidepressant and antianxiety effects more powerful than even commonly prescribed Prozac - all without psychedelic effects.
Why it matters
The discovery may present a path towards new kinds of antidepressants that are more effective and have fewer side effects than current medications, which don't work for many patients and must be taken daily.
Inspire treatments for addiction and depression
Used in some West and Central African religious ceremonies, the hallucinogenic ibogaine has shown promise as a potential treatment for substance use disorder and depression. Still, new medicines from the drug have been limited by rare but potentially deadly side effects, including causing dangerous irregular heartbeats.
What they found
Brian Shoichet, PhD, this time working with Anatomy Professor Allan Basbaum , PhD, and Pharmaceutical Chemistry Professor, Aashish Manglik , MD, PhD, designed and tested ibogaine-like compounds that could activate receptors in the brain linked to addiction and depression, while avoiding those behind ibogaine's mind-altering and harmful side effects. Molecules 1,000 times more potent than ibogaine on the serotonin transporter emerged and had anti-addictive properties in laboratory studies.
Why it matters
Nearly 50 million Americans were living with a substance use disorder in 2024. The work offers hope for new medicines to treat both depression and addiction, expanding the options to help ensure that everyone has access to treatments that work for them.
Solving psychedelics' biggest riddles
People have been excited about psilocybin therapy for depression, but it's been hard to tell how it compared to standard antidepressants.
The reason: The nature of psychedelics makes them difficult to study in a conventional "blinded" way, meaning the researchers nor the clinical trial participants know who received the medication or the placebo. "Blinding" helps ensure that patients' expectations don't influence how they report changes in their symptoms, potentially skewing results.
Because most patients know if they take a psychedelic, blinded studies haven't been possible, making it difficult to compare data to understand whether psychedelic therapy truly outperforms conventional depression treatment.
What they found
To help solve this, UCSF Translational Psychedelic Research Program clinical data scientist Balázs Szigeti, PhD, worked with colleagues at UC Los Angeles and Imperial College, London. In a first-of-its-kind approach , the trio compared data from psychedelic therapy trials with that from unblinded trials on antidepressants, in which researchers and patients knew they received antidepressants.
Why it matters
The results surprised researchers. Psilocybin worked virtually no better than common antidepressants. The finding, Szigeti cautions, doesn't mean psychedelic therapy doesn't work - rather just that it may not, generally, work better than traditional depression treatments. The study provides a more nuanced view of psychedelic therapy for depression and may guard against overly optimistic narratives about these medicines.

Saving Lives with Science
UCSF scientists discover treatments for the most heartbreaking and costly diseases, pioneer new industries, create jobs, and safeguard America.






