New research from the University of Copenhagen shows an increased risk of bacterial contamination in donated blood if the donor suffers from periodontitis. Still, it is considered safe to receive a blood transfusion, the researchers emphasize. However, the results indicate reviewing the screening approach.
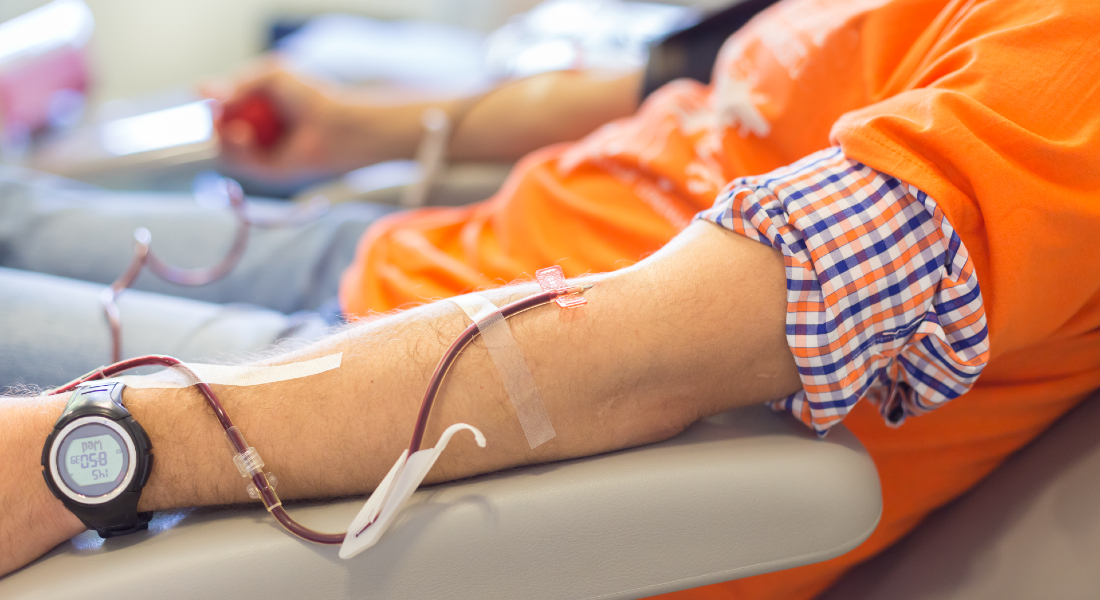
Each year, blood donors all over the world donate approximately 120 million portions of blood. Blood donations are important, because they save lives, but like many other treatments, in rare cases blood transfusion in itself can be the cause of an infection. In Denmark, all donor blood is screened for hepatitis and HIV to reduce the risk of transfusion-transmitted infection.
Now, a new study from the Faculty of Health and Medical Sciences at the University of Copenhagen and the Department of Clinical Immunology, Region Zealand, demonstrate that the risk of bacterial contamination increase if donors suffer from periodontitis. Interestingly, the results indicate that bacteria originating from the oral cavity evade the routine screening systems generally used.
Around half of the adult population above the age of 50 in the industrialized world suffer from periodontitis. In recent years, more and more studies link periodontitis to a number of diseases outside the oral cavity, including diabetes, cardiovascular disease and rheumatoid arthritis.
In the new study, the researchers demonstrate for the first time that periodontitis actually leads to increased risk of bacteria in blood donations. Interestingly, the bacteria remain undetected by the routine screening performed by the blood bank.
'Our results show a 6.4 times higher prevalence of viable bacteria in the blood donated by donors suffering from periodontitis compared to donors not suffering from periodontitis. That is a highly significant difference. It is noteworthy, that the bacteria are not detected by the screening system currently used in the blood bank, says Associate Professor, PhD Christian Damgaard from the Department of Odontology, Faculty of Health and Medical Sciences, University of Copenhagen.
'The presence of periodontitis implies having a large infected wound from which bacteria can enter the circulation. Every time you brush your teeth or chew food, the periodontal bacteria have direct access to the circulation.'
Bacteria are not detected by routine screening
The researchers have tested donor blood samples using different methods. They have used the exact same method as the blood bank using oxygen-rich incubation. Moreover, they have isolated the red blood cells and investigated growth using oxygen-free conditions. Using this approach, an important observation was made, Christian Damgaard explains.
'None of the samples studied bythe usual screening method showed bacterial contamination; thus, these products would have been approved for transfusion. On the contrary, when we studied the same samples using our more advanced method, we actually found viable bacteria in the blood', he says.
The risk of developing periodontitis increases with increasing age. Therefore, the researchers sampled blood from 60 different donors all above the age of 50. Around half of the donors turned out to have periodontitis.
Safe to receive donor blood
With this study, the researchers shed light on one aspect of the quality and control of donor blood, which may affect the risk of infections requiring hospital treatment. However, the researchers responsible for the study stress that they do not know, whether the observed bacterial growth has any clinical impact. Experience shows, that receiving donor blood is generally safe, says Susanne Gjørup Sækmose, Consultant Doctor at the Department of Clinical Immunology, Region Zealand.
'Patients can safely receive blood transfusions. In Denmark, we conduct around 360,000 blood transfusions a year, and infections due to blood transfusions are extremely rare - with less than one per year on average. In addition, we have a national system for monitoring side effects'.
The low incidence of infections caused by blood transfusions may be a result of the high level of safety. Also, the immune system will protect the patient from bacteria in the transfused blood. However, not all infections are reported to the blood bank. It is therefore important to identify risk factors that can lead to bacterial contamination, e.g. periodontitis - especially because donors do not necessarily consider periodontitis a factor worth mentioning when interviewed.
'In our experience, blood donors make sure to mention any diseases that may affect the quality of the blood. But few consider periodontitis a relevant disease; therefore, most donors probably do not mention it to the blood bank', says Susanne Gjørup Sækmose and continues:
'Our study suggests that we may have to develop new methods for efficient screening of donor blood in the future. But really, the most important point is to make sure that everyone sees the mouth as a part of our organism. Basically, diseases in the mouth may affect our overall state of health'.
The study 'Periodontitis increases risk of viable bacteria in freshly drawn blood donations' is published in the scientific journal Blood Transfusion.






