Published on
A team from UNIGE has designed a molecular system that distinguishes and neutralises cancer cells with unprecedented precision, paving the way for autonomous, self-regulating drugs.
How can cancer cells be targeted without damaging healthy tissue? This is one of the major challenges facing oncology today. Using synthetic DNA strands, a team from the University of Geneva (UNIGE) has created a "smart" system that can recognise cancer cells with exceptional precision and release powerful drugs only where they are needed. Beyond cancer treatment, this research paves the way to "smart" medicines and programmable drug delivery. The full article can be discovered in the latest issue of Nature Biotechnology.
The ability to directly target tumour cells with drugs is transforming cancer therapy, helping preserve healthy tissue and reducing the severe side effects associated with chemotherapy. Among the most promising approaches of recent decades are antibody–drug conjugates (ADCs), which use monoclonal antibodies to deliver therapeutic agents precisely to cancer cells. Despite their remarkable success, ADCs still face significant limitations, including poor penetration into tumour tissue and a restricted capacity for carrying drug payloads.
The drug itself can, in a simple way, 'compute' and respond intelligently to biological signals.
To address this issue, researchers at UNIGE have developed a new technology based on DNA strands. Because these DNA components are relatively small, they can move through tumours more easily than traditional antibody-based therapies, which can be bulkier and limited in how many drug molecules they transport.
More targeted and effective
In this new system, independent DNA strands carry distinct components, including two different cancer-targeting binders and a cytotoxic drug. When two specific cancer markers bind to their respective DNA-linked binders, the components self-assemble precisely at the tumour site. This assembly enables the delivery of higher drug concentrations, amplified by multiple DNA fragments snapping together where needed. Similar to two-factor authentication on a banking website, this process only occurs when both cancer markers are present. If either marker is missing, the hybridisation chain reaction cannot initiate, and the drug remains inactive.
In laboratory studies, the technology successfully identified cancer cells with specific combinations of surface proteins and selectively delivered potent drugs — while nearby healthy cells remained unharmed. The researchers also demonstrated that multiple therapeutics can be combined within the same treatment, a strategy that may help prevent or overcome drug resistance.
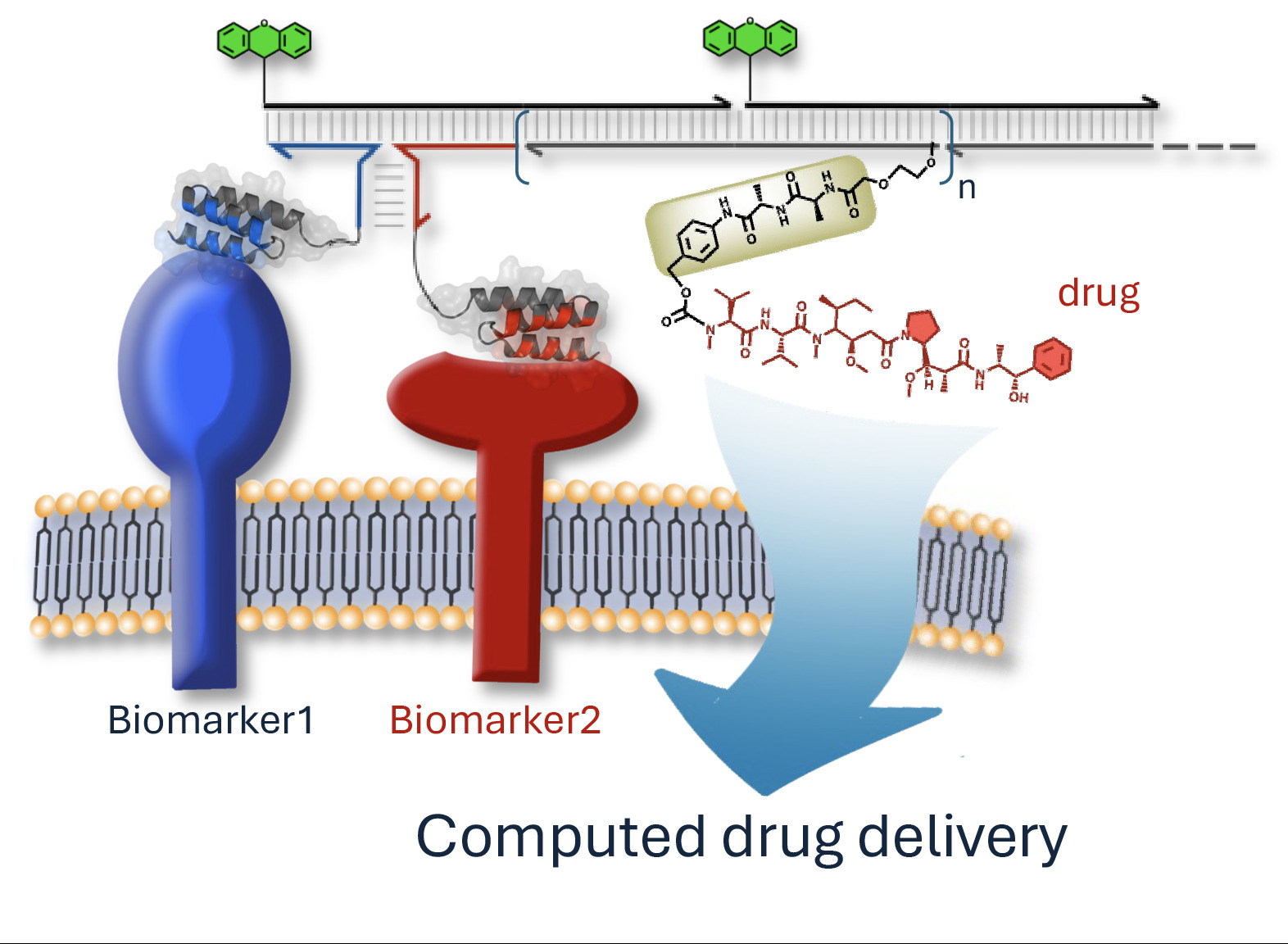 Smart DNA-based drugs. When the two "detectors" simultaneously recognize biomarkers 1 (blue) and 2 (red) on the surface of a diseased cell, the DNA fragments assemble like a puzzle and trigger a chain reaction that releases the drug into the center of that cell, while sparing neighboring healthy cells as much as possible. (Adapted from Figure 1 of the original article (Chen, S. K., López-Tena, M., Russo, F. et al. DNA–drug conjugates enable logic-gated drug delivery amplified by hybridization chain reactions. Nature Biotechnology, 2026).
Smart DNA-based drugs. When the two "detectors" simultaneously recognize biomarkers 1 (blue) and 2 (red) on the surface of a diseased cell, the DNA fragments assemble like a puzzle and trigger a chain reaction that releases the drug into the center of that cell, while sparing neighboring healthy cells as much as possible. (Adapted from Figure 1 of the original article (Chen, S. K., López-Tena, M., Russo, F. et al. DNA–drug conjugates enable logic-gated drug delivery amplified by hybridization chain reactions. Nature Biotechnology, 2026).
"This could mark an important step forward in the evolution of medicine, with the introduction of a self-operating drug system. Until now, computers and AI have helped us design new drugs. What's new here is that the drug itself can, in a simple way, 'compute' and respond intelligently to biological signals," explains Nicolas Winssinger, full professor in the Department of Organic Chemistry of the School of Chemistry and Biochemistry, Faculty of science, UNIGE, and last author of the study.
Like "computers"
Just as computers are built on simple logic operations, "and", "or", "not", this technology applies the same principle at the molecular level. In this first demonstration, an "and" logic gate ensures activation only when two cancer biomarkers are present, making the drug highly selective.
Looking ahead, future systems could integrate additional logic operations, creating medicines that behave like programmable systems, capable of complex decision-making inside the body. This opens the door to truly "smart" drugs that adapt to their environment, tailoring treatment to each patient's unique physiology while minimizing side effects. Rather than replacing human oversight, these innovations aim to make therapies more targeted and effective, offering new hope for personalized care and transforming the way we combat disease.
The research was supported by the Swiss National Science Foundation and builds on foundational work from the previous NCCR Chemical Biology program.






