For decades, multiple sclerosis research has focused on myelin, the insulation around the brain's wiring, which gets worn away in MS. Scientists paid less attention to another loss that was happening in parallel: neurons in the cortex, the seat of higher thinking and cognition, were dying.
A team from UC San Francisco, University of Cambridge, and Cedars-Sinai Medical Center now traces that loss to a breakdown in the DNA of neurons as inflammation overwhelms the brain. The finding helps explain why brain scans of people with multiple sclerosis (MS) reveal damage not only to white matter, the brain's wiring, but also to the brain's gray matter - and it points to a new direction for the field.
"It's become clear that in addition to promoting remyelination (rebuilding myelin) in progressive MS, it's essential to find ways to directly protect grey matter neurons themselves," said Steve Fancy , PhD, DVM, a professor in the UCSF Weill Institute for Neurosciences. He is the co-corresponding author of two papers that appeared April 1 in the same issue of Nature. "We can now point to a mechanism for why these vulnerable neurons in the brain are lost - DNA damage - and begin fighting MS on an entirely new front."
MS is typically diagnosed when clinicians see lesions in the myelin-rich white matter of the brain on MRI scans. White matter is made of the tails of nerves linking brain cells to one another, and it looks white on a brain scan.
The brain's grey matter, which houses the round "cell bodies" of neurons, can also have MS lesions, especially in its outer layers. These lesions are less common and harder to see on a brain scan, but they are a sign of chronic and disabling MS.
UCSF scientists found that brain cells die during multiple sclerosis when inflammation breaks their DNA. In an experiment in mice, they showed that similar neurons die when they lose the ability to repair their DNA. Images by Wenlong Xia, PhD, Fancy Lab, UCSF
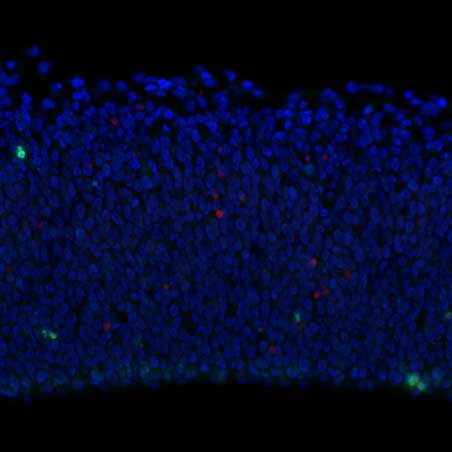
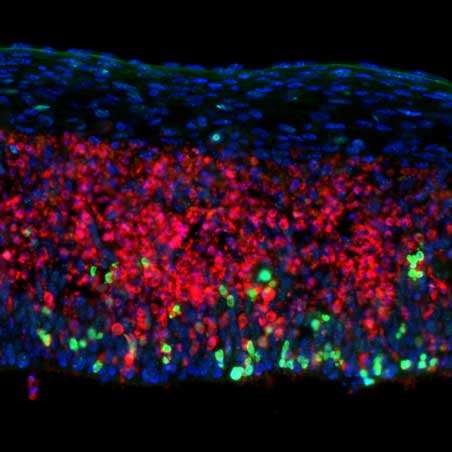
"We've had remarkable success developing therapies to slow the loss of myelin during MS, but grey matter lesions and the disability they cause have been harder to address," said Stephen Hauser, MD, the Robert A. Fishman Distinguished Professor in Neurology who directs the UCSF Weill Institute for Neurosciences.
This led scientists to focus on the neurons that die in these grey-matter lesions, which express a gene called CUX2. In the first study , they looked at developing mouse brains to see how CUX2 neurons are born. This occurs early in life, when the brain is growing quickly, putting cells under tremendous stress. The CUX2 cells rely on a mechanism to repair their DNA as they rapidly multiply, fan out into the far reaches of the brain, and wire up with one another. The mechanism depends on a stress-response gene called ATF4 to keep chromosomes intact. When the team removed ATF4, the growing neurons were rife with DNA damage, and this prevented the frontal part of the brain from forming.
"We saw that just a subset of its neurons were vulnerable to DNA damage," Fancy said. "And ATF4 is at the center of the strategy for surviving it."
In the second study , the team found DNA damage in grey matter lesions from people with MS involving the same CUX 2 neurons.
In mouse MS models, the researchers saw that inflammation sparked chemical reactions that damaged DNA in CUX2 neurons. The repair systems that protect these neurons from the stresses of development could no longer keep up; and this led to brain damage.
Together, the two studies outline the natural way the brain's outer layer neurons cope with DNA damage - and how that system breaks down in MS.
"The CUX2 neurons are like a 'canary in the coal mine' for the brain affected by MS," said David Rowitch, MD, PhD, deputy director for Research at Guerin Children's, professor of Paediatrics at the University of Cambridge, and co-corresponding author. "If we can protect these neurons, we might be able to contain the damage before the disease progresses."
Authors: Other UCSF authors include, Wenlong Xia, PhD; I-Ling Lu, PhD; Kimberly K. Hoi, PhD; Mingming Wei; Keying Zhu, PhD, MBBS; Xiao-Yan Tang; Julio Gonzalez Maya, MD; Vanesa Mattera, PhD; Sophia M. Panigrahi; Jennifer Ja-Yoon Choi; and Eric J. Huang, MD, PhD. For a complete list, see the paper.
Funding: National Institutes of Health (P01 NS083513, R35 NS137478, R01 NS128021, R21 NS133891, R01 NS124166, R01NS120981); European Research Council; Wellcome Trust; Dr. Miriam and Sheldon G. Adelson Medical Research Foundation; NIHR Cambridge Biomedical Research Centre; US Department of Defense; Alex's Lemonade Stand Foundation; Race to Erase MS; National MS Society; German Research Foundation; UK Dementia Research Institute; Therapeutic Innovation Networks; Hertie Foundation; Warren family; and the Spangler Foundation.






