History tells us that despite the global vaccine rollout, the end of the COVID-19 pandemic will be slow – and many new public health measures will become permanent. We may also have to live with the disease forever.

Small steps: It's a bumpy road to the moment we can throw our masks away, but for now, NSW residents can take solace in 28 days of no community transmission.
"It will be a long time before we can take international travel for granted, and some level of border restrictions will be in place for months and perhaps years to come," says Professor Janaki Amin, who heads Macquarie University's Department of Health Systems and Populations.
"The disease emerged so recently, and vaccines were developed very quickly, so there are still many unknowns," she says.
It's a bumpy road to the end of the pandemic, and we are likely to continue to see COVID-19 outbreaks for many years to come; she says that vaccines and low community transmission will turn the pandemic into a disease that is endemic, which we'll learn to live with.
Zero community infection isn't the end
Despite the lack of community infection, epidemiology historian Professor Peter Curson agrees we will never completely wipe out the SARS-COV2 virus that causes COVID-19.
"The only disease humans have eliminated throughout history was smallpox, which was done through widespread vaccination over decades," says Curson, who is Emeritus Professor of Population and Health at Macquarie University.
"But the diseases causing pandemics don't just disappear; most find a permanent reservoir in animals, making them almost impossible to eliminate," he says.
World Health Organisation investigators in China last week to trace the origins of the virus searched for an animal reservoir where the virus probably began – and likely still thrives.
Vaccines and low community transmission will turn the pandemic into a disease that is endemic, which we'll learn to live with.
Curson says that the COVID-19 pandemic challenged prevailing beliefs that humans have won the battle against infectious diseases.
"Epidemics and pandemics do fade away over time, but they are never truly gone, largely because humans ignore the nature of the biophysical environment and the significance of how bacterial and viral infections are nurtured in our world and how they evolve and mutate," says Curson.
Even the plague – spread by fleas containing the Yersinia pestis bacteria and responsible for killing around a third of the world's human population in the mid-1300s – has survived in large natural reservoirs around the globe, killing more than 200 people in an outbreak in Madagascar in 2017.
How we return to 'normal'
"Everyone wants to know when we can return to normal, but there are no easy answers," says Amin.
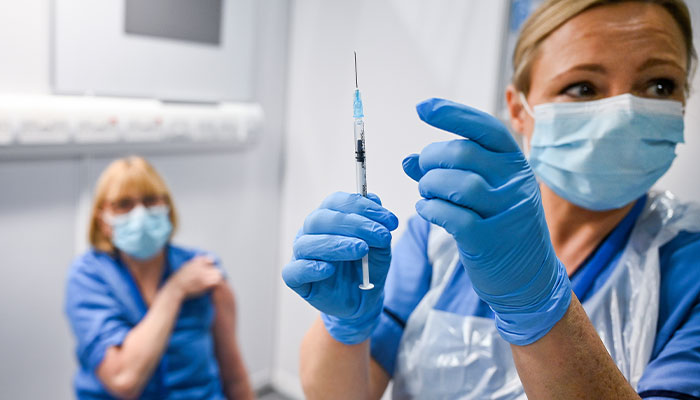
Unprecedented: The speed of the global response, including the development of vaccines, separates it from past pandemics, says Professor Amin.
Pursuing a 'no community transmission' strategy via tight border restrictions and quarantine has been hugely effective in Australia, she says, but it has meant losing our free interaction with the outside world.
"Many countries face massive levels of disease and death with overwhelmed health systems while Australians have been relatively free from this – but it will be a long time, maybe years, before we can travel freely."
She says that 'travel bubbles' with other countries that are free of community transmission are the likely way that borders will begin opening up.
Ongoing restrictions could include proof of vaccination before travel, and even quarantine from countries where there are outbreaks.
Speed of transmission and response has no precedent
Amin says that while history is always a useful guide, the speed of transmission of COVID-19 and the magnitude of the global response, separates it from past pandemics.
"The virus spread and turned into a pandemic faster than ever before, and we're now trying to turn it around really quickly, creating multiple vaccines within a year, some with 95 per cent efficacy against disease, which has never been done before," she says.
There are big, big unknowns about reinfection, and about how many times we'll need to be vaccinated.
She adds that COVID-19 can't be directly compared to an influenza epidemic. Fatality rates are higher, and there are also long-term chronic health complications for survivors which we are just beginning to understand.
The speed of infection, and speed of response, has left us with huge knowledge gaps, she says – and that makes it really difficult to develop policy or make predictions about what will happen next.
"There are big, big unknowns about reinfection, about how many times we'll need to be vaccinated, and we still only have very limited information about whether vaccination will prevent transmission," Amin says.
States' struggles are nothing new
Since colonisation, Australia has dealt with more than 20 pandemics – including HIV-AIDS, polio and three influenza pandemics last century – and more than 35 major epidemics, says Curson.
While this pandemic has moved faster and seen quicker responses than ever before, current issues around interstate and international border closures are nothing new.
"The Commonwealth Government and the states and territories have always struggled to understand the origin and the means of spread of epidemics and pandemics and have fought with each other over the best way to address the outbreak," Curson says.
"We've seen control and containment plans over time which led to escalated fear and the institution of quarantine and refugee camps to stop the movement of people."
Curson says that the key to the control of a pandemic is not simply vaccination, or government regulations, but also the way people perceive the risk of disease and respond with their actions.
International travel and large-scale events will return when the population begins to feel safe, he says.

Professor Janaki Amin (pictured) is Head of the Department of Health Systems and Populations.
Professor Peter Curson is Emeritus Professor of Population and Health in the Faculty of Medicine, Health and Human Sciences






