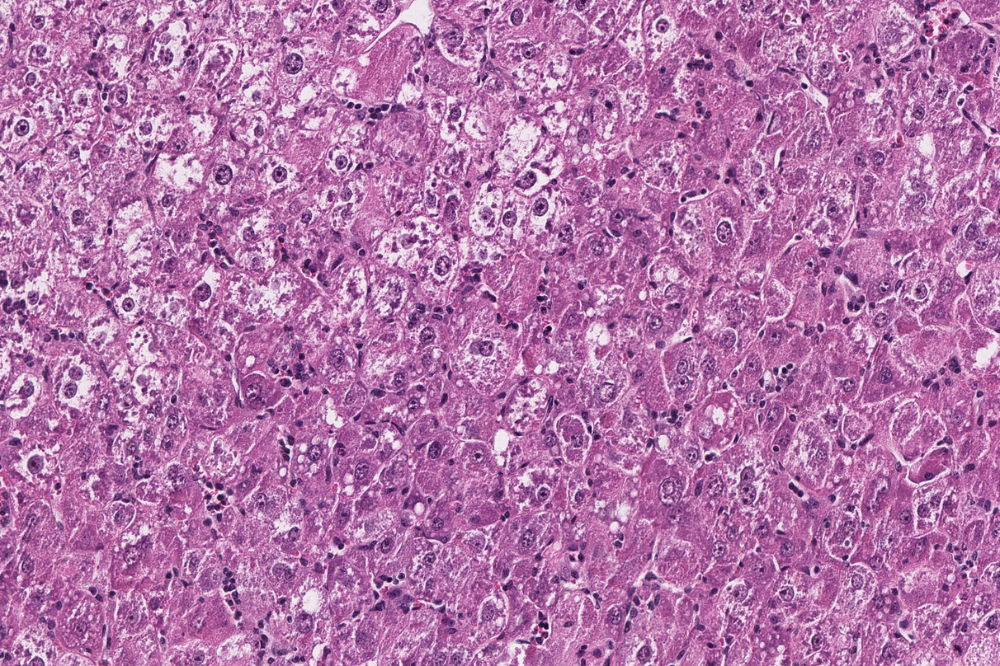
Histological image of a tumor from the first mouse model in which chronic viral infection progresses to liver cancer, closely mirroring what happens in people with hepatitis C. (Credit: Rice Lab)
Liver cancer is one of the world's deadliest cancers, and most cases are linked to chronic viral hepatitis. Yet scientists have lacked an animal model that faithfully recapitulates how the disease unfolds in people, from initial infection with a virus to liver inflammation, scarring, and cancer.
Now, researchers at The Rockefeller University have developed that model, as described in the Journal of Hepatology. By infecting ordinary laboratory mice with an engineered version of Norway rat hepacivirus (NrHV)-a close relative of hepatitis C virus (HCV)-and tracking the animals over 18 months, the team documented the progression from chronic viral hepatitis to spontaneous liver cancer.
"This model fills a critical gap that has long existed in the field," says Charles M. Rice, whose Laboratory of Virology and Infectious disease helmed the study. "For the first time, we have a system in which natural chronic viral infection drives liver cancer in an immunologically healthy animal, opening the door to studies and preclinical trials that simply weren't possible before."
A surrogate for hepatitis
Hepatocellular carcinoma (HCC) is the most common form of liver cancer and the third leading cause of cancer death worldwide. More than 75% of people who develop HCC have a chronic infection with hepatitis B virus (HBV) or hepatitis C virus (HCV). These infections are known to lead to ongoing liver inflammation and scarring but how they ultimately trigger HCC is not fully understood.
Since hepatitis viruses are highly species-specific, scientists have been hampered by the inability to infect mice with the human virus to study how chronic infection progresses to cancer. Some researchers have tried adapting the virus, engineering mouse liver cells to contain human proteins, or transplanting human liver tissue into mice, but none of the models fully mimicked the full arc of hepatitis-driven HCC.
The path forward came from New York City rats. About a decade ago, researchers at Columbia University discovered NrHV circulating in the city's rat population. NrHV is closely related to HCV and naturally infects rats' liver cells. Earlier work from the Rice lab established that NrHV could infect laboratory mice leading to liver inflammation resembling that seen in humans with HCV.
The logical next question was whether chronic NrHV infection would drive the same kind of progressive liver disease seen in patients.
"The central question was whether chronic viral infection alone, without any additional genetic manipulation or chemical insult, could take mice all the way from hepatitis to liver cancer," says first author Mariana Nogueira Batista, a research associate in the Rice lab. "The answer turned out to be yes."
From infection to cancer
To establish persistent infection, the researchers temporarily suppressed the animals' immune systems. This allowed the virus to take hold; the immune systems then recovered and remained intact for the rest of the 18-month study.
What followed closely tracked the course of chronic HCV in people. Infected mice developed liver inflammation patterns that closely mirror those seen in human disease, including distinctive clusters of immune cells in the liver that are considered a hallmark of HCV. Liver scarring steadily progressed over the following months. By 18 months post infection (equivalent to a human in their 50s or 60s), 67 percent of infected mice had developed HCC, compared to just 4 percent of uninfected controls, and the tumors resembled those seen in humans with HCV-associated human liver cancers.
"This is not just a model of hepatitis-it's a model of the full disease continuum," Batista says. "Chronic infection, scarring, and cancer all develop spontaneously, in sequence, without any chemical manipulation or engineered cancer-causing mutations."
Male mice were more than twice as likely to develop HCC than females, mirroring the sex disparity in the cancer in humans. And some mice that spontaneously cleared the virus yet still went on to develop cancer, echoing elevated cancer risk even in people who have been cured of hepatitis C.
A platform for new therapies
Because the mice have intact immune systems and the course of liver disease so closely mimicked what is seen in humans, the new animal models represent a leap forward for researchers to study exactly how viruses and the immune system work together to trigger HCC.
"We don't fully understand what the virus contributes and what the immune system contributes to disease development," Batista says. "Now we have a model to start answering those questions."
The mice can be used, for instance, to test immune-based therapies currently used to treat HCC, to understand why these treatments work in some patients and fail in others.
Rice's group plans to carry out both basic research on the early stages of HCC to identify biomarkers for cancer diagnosis and explore the effects of current and new experimental therapies.






