Scientists at Hokkaido University and collaborators have identified how inflammatory changes in tumors caused by chemotherapy trigger blood vessel anomalies and thus drug-resistance, resulting in poor prognosis of cancer patients. Through mice experiment, the team also found that the combined usage of an inhibitor and anticancer drug makes chemotherapy more effective.
Chemotherapy is often chosen for treating inoperable cancers, such as locally advanced and metastasis cases. It is, therefore, essential to unravel drug-resistance in this treatment, which has been a major factor in making cancer malignant and causing metastasis.
Tumor blood vessels play a key role in cancer progression because they carry nutrients and oxygen to tumors and serve as pathways for metastasis. It had been generally believed that tumor endothelial cells (TEC) lining tumor blood vessels did not acquire drug-resistance. However, several years ago, the group's mice experiments showed TEC can obtain various anomalies, suggesting blood vessels, as well as cancer cells, can contribute to making tumors drug-resistant. For example, the group demonstrated for the first time that TEC in blood vessels resist paclitaxel - a chemotherapy medication used for second-line treatment of urothelial cancer - due to the expression of ABCB1 which pumps out the drug from blood vessels.
However, much remains unknown about how human blood vessels are involved in cancer acquiring drug-resistance.
To help unravel this mystery, the group first analyzed tumor tissue samples from urothelial cancer patients before and after they underwent first-line chemotherapy. They found ABCB1 expression was increased in TEC in blood vessels of more than 60 percent of patients who received chemotherapy, and that their prognoses were poorer than patients whose ABCB1 expression remained the same after the treatment.
In addition, they analyzed TEC in blood vessels and bladder cancer cells to study how chemotherapy affects ABCB1 expression. The results showed that the increased secretion of interleukin-8 (IL-8) in cancer cells after chemotherapy caused inflammatory changes, increasing the ABCB1 expression in TEC. In another experiment, mice with urothelial cancer administered with the ABCB1 inhibitor together with paclitaxel showed suppressed formation of new blood vessels and thus metastasis to the lung.
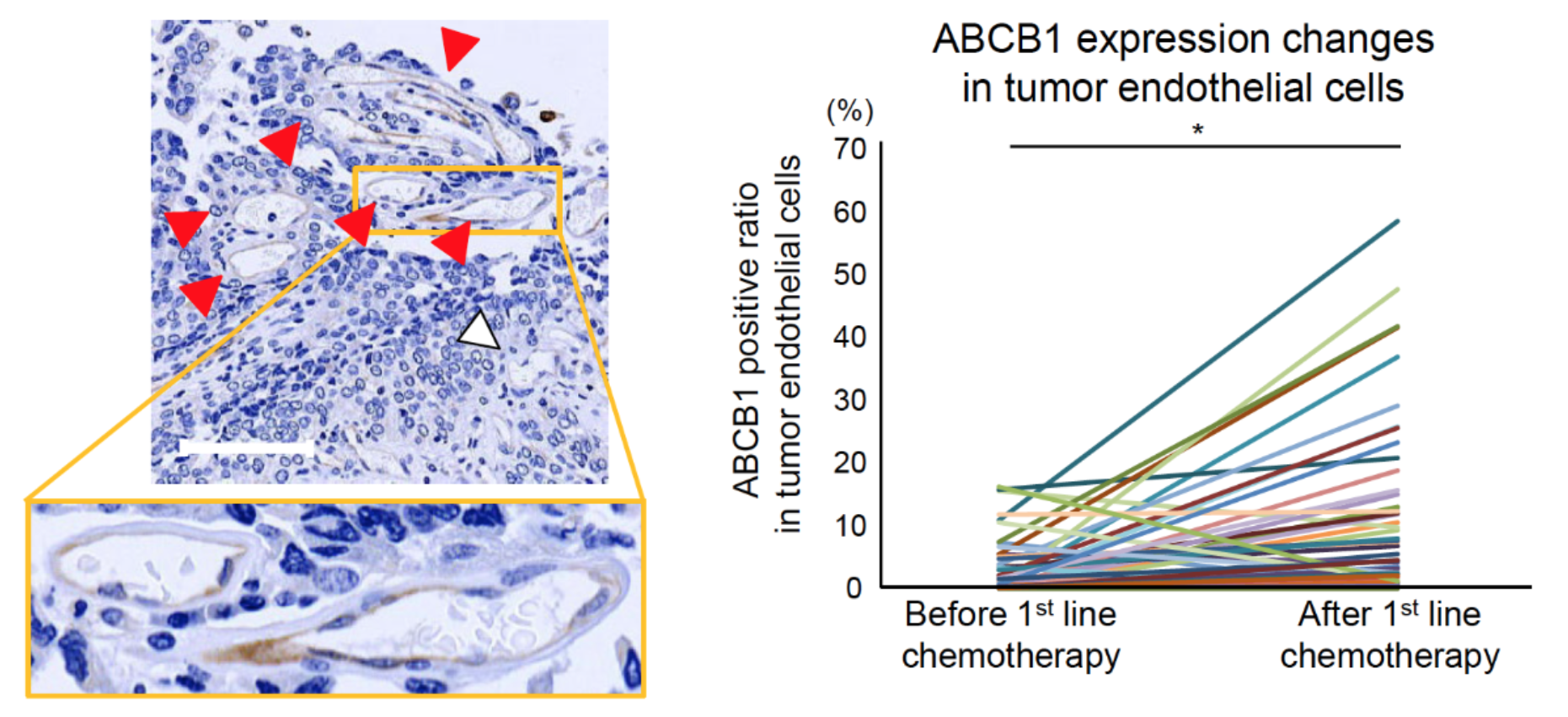
(Left) ABCB1-positive blood vessels (brown) after first-line chemotherapy in human urothelial carcinoma. Red and white arrowheads indicate ABCB1-positive and negative blood vessels, respectively. (Right) ABCB1 expression was increased in tumor blood vessels of more than 60 percent of patients who received chemotherapy. (Kikuchi H., et al., Cancer Research, June 15, 2020)
"Our study provides evidence, for the first time in humans, that inflammatory changes in tumors can cause drug resistance in cancer blood vessels," says Kyoko Hida of Hokkaido University who led the group. "These findings could help devise new treatment strategies, such as the development of inhibitors targeting ABCB1 and IL-8, to suppress drug resistance and improve prognosis."

Kyoko Hida (left), Hiroshi Kikuchi (Second from the right), Nako Maishi (right) of the research team at Hokkaido University
Original article:
Kikuchi H., et al., Chemotherapy-induced IL-8 upregulates MDR1/ABCB1 in tumor blood vessels and results in unfavorable outcome, Cancer Research, June 15, 2020.
DOI: 10.1158/0008-5472.CAN-19-3791
https://cancerres.aacrjournals.org/content/early/2020/06/10/0008-5472.CAN-19-3791






