Professor Tetsuya Yamada and his team members are tackling diabetes - widely regarded as a national affliction in Japan - by investigating ways to raise basal metabolic rate and enhance the burning of fat and sugar, guided by insights from the functions of female brown adipose tissue. They are also developing an AI model to detect super-early prediabetic conditions.
Humans have the ability to maintain a stable internal environment to prevent body temperature from dropping in cold conditions. This is made possible by signals from nerves and chemical messengers that transmit instructions throughout the body, finely tuning blood pressure, body temperature, and heart rate. This regulatory mechanism is known as homeostasis. The autonomic nervous system and the endocrine system play central roles in making these adjustments, controlling tissue functions through hormones that circulate in the bloodstream and autonomic nerves that extend throughout the body.
Abnormalities in endocrine function can lead to various illnesses, with diabetes as a notable example. In healthy individuals, the pancreas secretes a hormone called insulin when blood glucose levels rise after a meal. Insulin binds to insulin receptors on cells, allowing them to absorb glucose from the blood and maintain steady blood glucose levels. However, when there are abnormalities in insulin action, cells are unable to take in glucose, resulting in its accumulation in the blood and a failure to deliver essential energy (glucose) to the body. Consequently, individuals not only experience malnutrition but may also develop atherosclerosis (hardening of the arteries) due to excess blood glucose, triggering complications such as myocardial and cerebral infarctions.
There are two types of diabetes. The first is Type 1, which occurs when the pancreas cannot secrete insulin because the immune system attacks and destroys the insulin-producing cells for an unexplained reason. This type of diabetes can develop in people of all ages, including the young. Patients with Type 1 diabetes often experience significant surges in blood glucose levels and malnutrition, leading to drastic weight loss and severe fatigue. The second type is Type 2, which is often caused by obesity. Accumulated fat impairs the function of insulin receptors and their downstream signaling pathways in cells, making it difficult for glucose in the blood to be absorbed. Following a pre-diabetic phase - during which lifestyle changes and a healthy diet can prevent disease progression - the condition may gradually worsen.
In Japan, it is estimated that one in six adults is either diabetic or pre-diabetic. Leading the fight against what can be considered a national affliction is a research team that includes Professor Tetsuya Yamada, who is exploring possibilities for diabetes treatment and prevention while engaging in both clinical and research work. We spoke with Professor Yamada about the research paving the way for improved diabetes treatment and prevention in the future.
Pick up
- Blood sugar (glucose) as the body's energy source
- This energy increases through eating. Carbohydrates that are consumed are broken down and absorbed in the small intestine, allowing glucose to enter the bloodstream.
- Insulin: A hormone closely associated with diabetes
- Insulin, a hormone secreted by the pancreas, is released when blood glucose levels rise. It helps control blood glucose levels by facilitating the delivery of glucose to cells. When insulin is not secreted properly due to immune abnormalities, or when its function is compromised by obesity, blood glucose remains elevated in the bloodstream. This can result in atherosclerosis and various other health issues.
- Transferring sugar (glucose) from blood vessels to cells
- Insulin binds to a protein known as the insulin receptor, allowing blood glucose to be absorbed from the blood vessels into the cells. This process lowers blood glucose levels and provides energy to the cells.
"Human life-sustaining mechanisms are fascinating precisely because they're full of mysteries"

Diet as a path to treating diabetes; Insights from women's metabolism
When people think of diabetes treatment, insulin injection or medication usually comes to mind. Raising insulin levels to lower blood glucose is essential for people with Type 1 diabetes, who lack insulin, and can also help people with Type 2 diabetes, whose insulin function is impaired. For many Type 2 patients whose condition is largely linked to obesity, a healthy diet is highly effective. Reducing body fat can restore insulin sensitivity, so I advise my patients to reassess their lifestyle habits. Weight loss, however, does not happen overnight, so in my clinical practice we have explored ways to reduce obesity with less burden on patients.
While appetite-suppressing weight-loss drugs are already available on the market, our research focuses on basal metabolic rate (BMR), the energy required to sustain essential functions such as breathing and maintaining body temperature. BMR peaks in the teenage years and then declines with age. We hypothesized that raising patients' BMR would promote weight loss by increasing energy expenditure even if their diet and activity levels remained the same.
Among the components that contribute to BMR, brown adipose tissue (BAT) plays a major role in thermoregulation. BAT raises body temperature by burning fat and has thus attracted attention as a promising target for obesity prevention and treatment. Research so far shows that BAT is more active in women than in men, resulting in higher energy expenditure. Believing that uncovering the mechanisms for this sex difference would provide insights into how to raise metabolic rate, we launched this research.
Mitochondria - the body's energy source - hold the key to sex differences in energy expenditure
BAT is rich in mitochondria[1], organelles that produce heat. Mitochondrial activity is regulated by a protein called PGC-1α. We examined male and female mice and found that females have higher PGC-1α levels and larger mitochondria. We also found sex differences in PGC-1α function.
We used male and female mice lacking PGC-1α and compared the effect on mitochondrial heat production. We found that only female mice were greatly affected, indicating that PGC-1α influences heat production primarily in females. Further research showed that PGC-1α regulates phospholipid synthesis[2] in membrane that underlie mitochondrial heat production, and that the female hormone estrogen enhances PGC-1α function. By these multiple mechanisms, BAT is more active in women than in men.
Pursuing research on female BAT may ultimately lead to drugs that boost BMR and strategies that help prevent obesity. It may also clarify why women - particularly premenopausal women - are less likely than men of the same age group to develop diabetes. This research is also expected to contribute to gender-specific medicine[3].
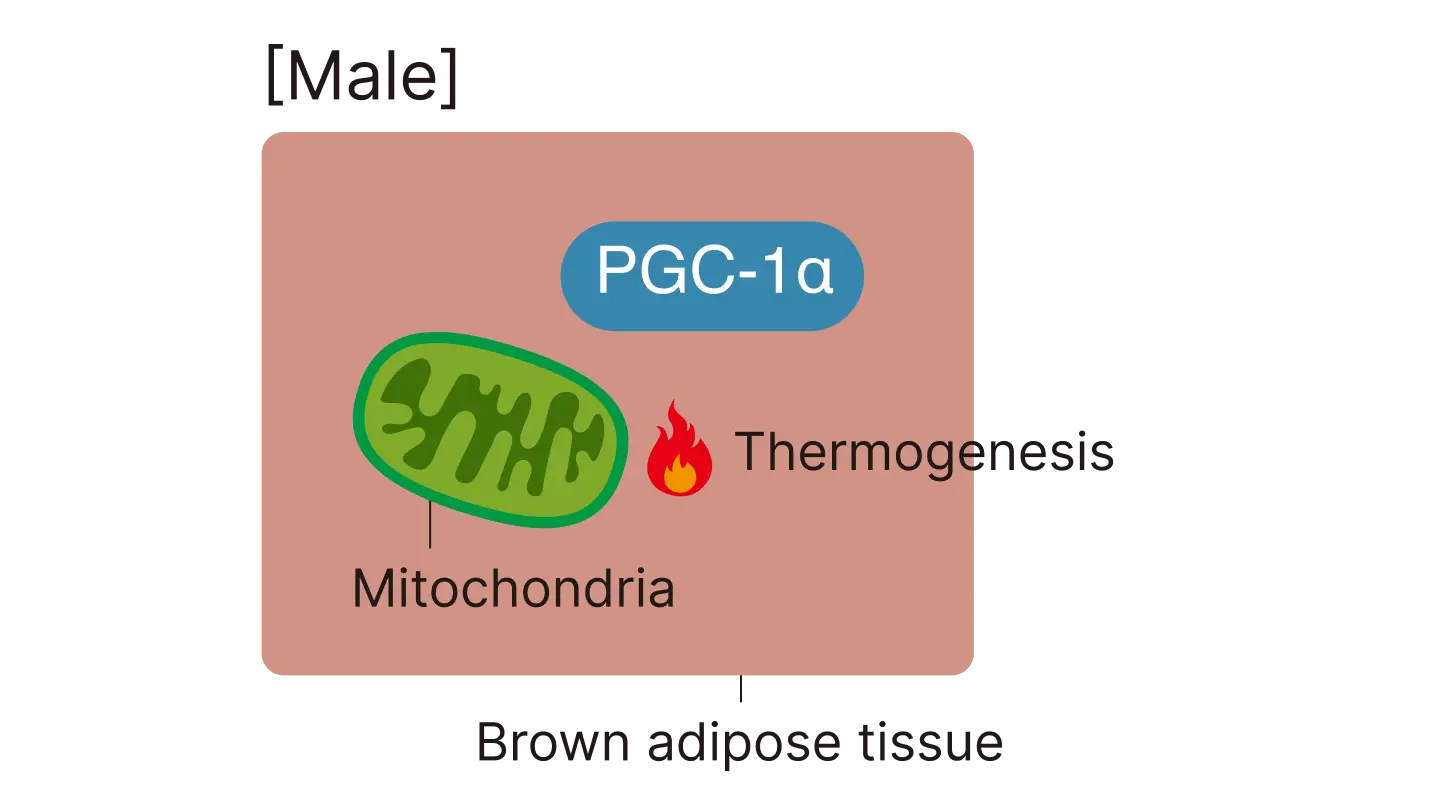
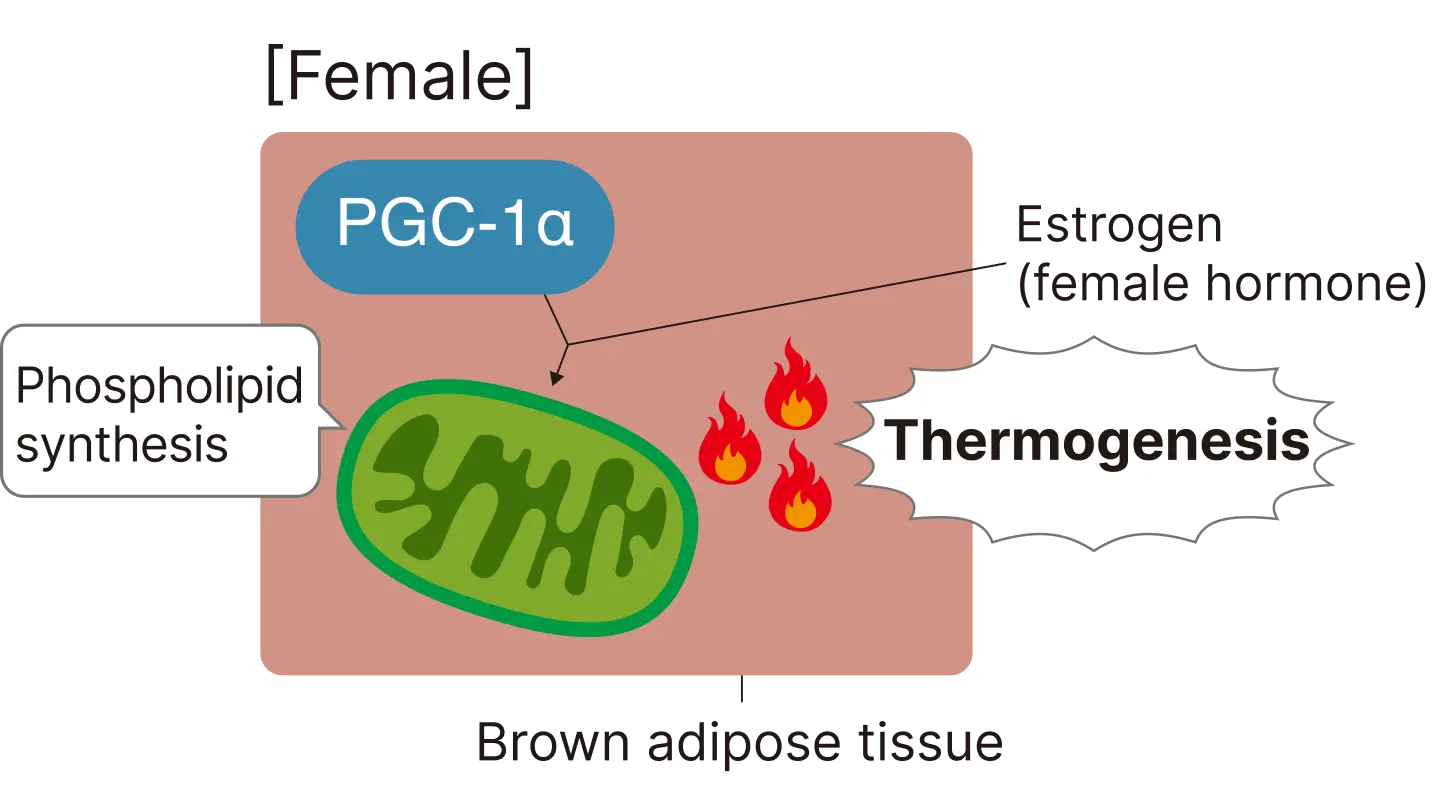
Differences in BAT-mediated calorie expenditure between male and female mice
PGC-1α in male mice does not significantly affect mitochondrial structure, whereas in female mice it does. In females, PGC-1α promotes the formation of comb-shaped folds (cristae) in the mitochondrial membrane - phospholipid-rich structures that support heat production - thereby enhancing thermogenesis. This function is promoted by estrogen.
Overturning conventional wisdom with AI: Toward next-generation medical examination and treatment
Preventing diabetes progression is as important as treating it. In particular, Type 2 diabetes can be prevented in people with prediabetes by changing lifestyle habits, so early detection is crucial. Yet prediabetes often goes unnoticed because its symptoms are subtle, and diagnosis requires blood tests, leading to delays in detection.
The situation has prompted our research team to develop a novel AI model, DiaCardia, that can detect prediabetes simply by analyzing an electrocardiogram (ECG). The model can automatically determine whether a person is prediabetic from an ECG and therefore could also be applied to data from watch-type wearable devices, enabling diagnosis through a simple procedure. Of course, accurate diagnosis still requires clinical testing at a medical facility, but the AI offers a rapid method to detect early signs of the disease. We are continuing this research with the goal of practical application.
We are developing this model based on the idea that expertise in AI and engineering is valuable for research. This project was initiated before the merger of Tokyo Medical and Dental University with Tokyo Institute of Technology. Now, one year after the merger, we have observed that the barriers between academic disciplines have significantly decreased. I believe that the integration of medicine with AI, engineering, and other fields will continue to accelerate.
Conceptual image of measuring an electrocardiogram using a wearable device
By touching the device with a finger of the opposite hand to the one wearing it, an electrocardiogram can be measured. Looking ahead, it is anticipated that anyone will be able to detect whether they are prediabetic by using a wearable device equipped with the DiaCardia AI model app.

"We often encounter unanswered questions in medical examinations, treatment, and research. However, inspiration derived from thorough reflection and the diverse ideas of team members can lead to tangible results"
The moment when the perspectives of clinician and researcher align
Why is this treatment not working? Why is this drug ineffective? Each question we face as physicians drives our research themes and motivates our team. We contemplate various questions daily and often arrive at solutions based on our observations and experiences, discovering connections between phenomena that initially seemed unrelated. These unexpected linkages inspire us. However, inspiration cannot occur without thorough preparation. I believe that a research team can achieve innovative results only when each member actively pursues knowledge about medical care and the human body, leaves no question unaddressed, and allows their ideas to converge. It is our sincere hope to value each member's free ideas while making discoveries that will ultimately benefit the health of many patients.
Glossary
- [1]
- Mitochondria:These organelles are found in almost all cells and contain unique DNA that differs from nuclear DNA. They burn fats and sugars to synthesize ATP, an energy molecule essential for life-sustaining cellular activities. UCP-1, which is selectively present in the mitochondria of brown adipose tissue (BAT), uncouples ATP synthesis, dissipating energy as heat in the process.
- [2]
- Mitochondrial phospholipid synthesis:Mitochondria have a double-membrane structure composed of lipids. The inner membrane, where ATP is synthesized, has a cristae structure (numerous folds). Phospholipid synthesis increases the formation of cristae, thereby enhancing the efficiency of ATP synthesis.
- [3]
- Gender-specific medicine:Gender-specific medicine is an approach to medical care that takes into account biological, social, and cultural differences between genders. It aims to provide more accurate diagnoses, treatments, and disease prevention strategies by considering differences in disease incidence, symptoms, and drug effects between genders.






