TSU neuroscientists studied the processes that occur in a total disturbance of the blood supply to the brain in the hippocampus - a portion called the memory manager. The immune cells of the central nervous system try to save it by breaking nerve connections and suppressing the hyperexcitation of neurons, their so-called excitotoxicity. New fundamental data are important for effective approaches to the prevention of cerebral ischemia in people at risk, for example, with severe cardiac pathologies. The research results were published in the highly-ranked International Journal of Molecular Sciences.
- Despite the importance of damage to the hippocampus, the features of damage to this section during cardiac arrest in humans and the time of occurrence of these injuries are poorly understood, - says Tatyana Ananyina, a co-author of the article and a staff member of the TSU Laboratory of Neurobiology. - We tracked these changes in a model of total ischemia in rats that suffered cardiac arrest for seven minutes. The most serious disorders occur precisely in the hippocampus because excitation from a huge number of neurons from other areas of the brain comes into this zone.
The hippocampus is responsible for the process of remembering meaningful information. It is sometimes referred to as a 'memory manager'. The formation of emotions, navigation, and much more depend on the state of this department. By comparing new signals with memories stored in the hippocampus, the brain decides whether to remember new information.

Along with the predictable events (death of neurons, inflammation, and others), we recorded a decrease in the level of myelin, an important component of nerve fibers, the state of which determines the speed of propagation of electrical impulses between neurons, - says Marina Khodanovich, head of the TSU Laboratory of Neurobiology. - With a total disturbance of the blood supply to the brain, numerous SOS signals are sent to the hippocampus from its different parts of the brain. The neurons receiving them cannot cope and the overload leads to their death.
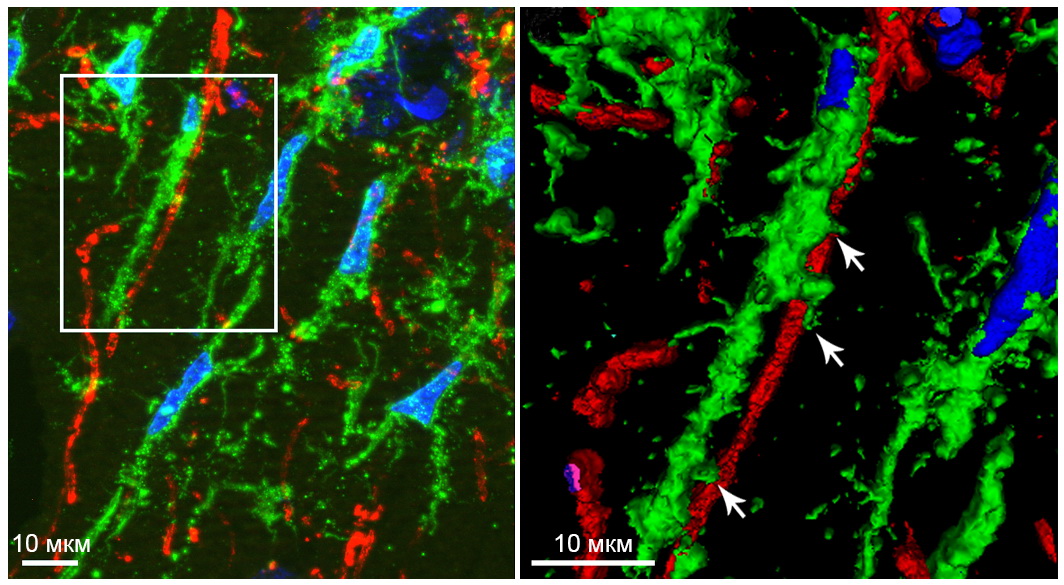
However, the body is trying to prevent this, and microglia, the immune cells of the brain, intervene in the situation. They not only fight pathogens and absorb the remains of dead cells, but also provide plasticity. In rodents that underwent total ischemia in the experiment, the microglial cells acquired a specific appearance - they extended into a rod-shaped form and were located along with the myelinated processes.
Presumably, microglia of this shape destroy synaptic contacts for disconnecting the neural network and stopping the flow of external signals, the excess of which is fraught with the death of neurons in the memory center.
- It is known that microglia are capable of interrupting communication between neurons and rebuilding neural connections. Such a process, for example, occurs when a person grows up, but in the case of cerebral ischemia to the protection of the hippocampus, this functionality has not yet been studied, says Marina Khodanovich. - Studies have shown that on the 10th day after the temporary cessation of blood circulation, the microglia are still making attempts to protect the hippocampus, but on the 30th day, they no longer do. During this period, they are only engaged in clearing - utilization of dead cells' stumps.
At the same time, scientists were able to trace other changes that occur in the damaged area. On the 30th day, there is a significant increase in the precursors of oligodendrocytes - cells that provide myelination.
Having matured, oligodendrocytes begin to work to restore myelin in bare axons - processes along which impulses are transmitted from one neuron to another. The fundamental data obtained by scientists, in the future, can be a basis for new approaches to the therapy of patients after cardiac arrest or cerebral stroke.






