is a rampant chronic disease affecting more than 37 million Americans. In California, nearly half of adults have either undiagnosed diabetes or are prediabetic. People with diabetes are at risk of developing diabetic ulcers, a painful and costly complication of poorly managed diabetes. To learn more about how to prevent and treat diabetic ulcers, we interviewed Distinguished Professor Roslyn Isseroff, a dermatologist at UC Davis School of Medicine and chief of dermatology at VA Northern California Health Care.
What are diabetic ulcers and what causes them?
Diabetic ulcers are a serious complication caused by a combination of poor circulation, susceptibility to infection and nerve damage from high blood sugar levels. When there is limited blood flow to the wounded area, the body struggles to heal its skin wounds. So, these wounds develop into diabetic ulcers.
Diabetic ulcers are more prevalent among the diabetic elderly. It is estimated that a quarter of people with diabetes will develop a foot ulcer at some stage. Unfortunately, a quarter of those with ulcers might end up with amputations.
How long do diabetic ulcers take to heal?
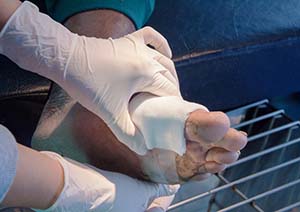
Diabetic ulcers are longstanding problems. Even with the best standard treatment, about 50% of patients don't completely heal in 12 weeks. We basically see the patient once a week to check their wound and remove the diseased or dead tissues, a procedure known as debridement. We also apply topical bandaging and treatments and sometimes use advanced therapies like bioengineered skin.
Still, treating chronic wounds, especially diabetic ulcers, takes a long time. We see our patients for many months. Even when they heal, there's a pretty high chance of recurrence. In some cases, the wound might not heal well and gets infected. The body tissues die, and this can lead to gangrene.
How should people with diabetes take care of their skin to prevent ulcers?
People with diabetes are advised to:
- Regularly check the body, especially the toes and the ball of their foot, for any cuts
- Don't delay treatment of any wound, no matter how minor
- Take the pressure off the wounded area
- Clean and cover the wound with the proper dressing
Tell us about the skin-brain connection. How do chronic wounds relate to behavioral and cognitive changes?
Our research, for the first time, uncovered a skin-to-brain signaling pathway. It showed that the wound itself could cause subsequent central nervous system and behavioral changes.
We, and others, have observed behavioral and cognitive changes in our patients who have chronic wounds. It is unknown if the wound causes these changes, or they are just associated findings. The idea we proposed is that when a patient gets a wound that heals right away, there is not much sustained signaling of stress to the brain. But a chronic wound keeps activating the sensory receptors for painful stimuli (known as nociceptors), sending a more continuous skin-to-brain relay. This continuous flare generates brain signals of stress that are translated into behavioral changes.
We carried out research in mice and found that skin wounds result in a relay to the brain. This relay leads to the activation of stress markers, alteration of inflammatory mediators and changes in behavior and cognition. Mice with wounds showed more signs of despair and impaired memory than those with no wounds.
We often see similar behavior in patients with chronic wounds that need daily wound care. Some seem unable to attend to their wounds despite the serious risk of losing their foot to amputation. We also observe depression and cognitive disability reflected in the perception of inability to take care of their wounds. Some even seem to be disassociated from the reality of the serious nature of this problem.
How does this insight about the skin-brain connection translate into clinical care for patients with chronic wounds?
As physicians who treat chronic wounds, we generally don't assess the mental status of our patients. We often just focus on healing the wound. We can be more aware of the patients' mental health and recommend intervention if they show depression or cognitive disability.
Ideally, we should have mental health specialists in our clinics to address the mental health needs of patients. Patients need additional education on how their mental health can affect their healing, and conversely, how the non-healing wound may be affecting their mental health. These interventions could help the overall healing process and result in better outcomes for our patients with chronic wounds.
To learn more about Isseroff's study on skin-brain connection, read her article in Brain, Behavior, and Immunity- Health.
10 steps to prevent diabetic foot ulcers
- Manage your blood sugar
- Trim your toenails and file down sharp edges
- Keep feet clean, dry and moisturized
- Wear cotton socks to keep feet dry
- Wear comfortable, proper-fitting closed-toe shoes
- Leave growth removal to your doctor
- Cover your feet, and don't go barefoot, even indoors
- Eat a healthy diet rich in protein
- Stay active
- Stop smoking






