Nittany, a blue fawn Great Dane, was only seven months old when she first collapsed. The puppy was suffering from a condition that causes the heart to beat abnormally, called a ventricular arrhythmia. It's a common and often deadly condition in dogs, but the cure - cardiac ablation - is so specialized that few veterinary hospitals have the training and expertise to perform it.
"Cornell is one of only two places in the country that is regularly prepared to offer this procedure," says Dr. Weihow Hsue, assistant professor in the Section of Cardiology at the Cornell University Hospital for Animals, who co-led Nittany's care team.
When owners Brandi and Michael Gwin of DuBois, Pennsylvania, learned that Cornell could help Nittany's heart, they brought her in for treatment.
"Nittany is a big, goofy, loving dog that doesn't know her own size," says Brandi Gwin. "After Nittany was diagnosed, she spent a lot of time sleeping. She still went to doggie daycare but would tire out easily."
Electro-anatomical mapping
Ventricular arrhythmias are one of the most common abnormal heart rhythms in dogs. Instead of beating steadily, hearts with this condition operate in one of two extremes: either a faltering stutter or a persistent, overwhelming string of heartbeats. Both wear on the heart and cause lethargy, but the latter can also lead to collapse and even sudden death.
"In healthy hearts, a normal rhythm begins in the sinus node, progresses through the upper chambers and then activates the lower chambers, called ventricles," Hsue says.
For hearts suffering from ventricular arrhythmias, that rhythm begins in the lower chambers instead. This is often due to structural heart disease. But for some animals, including Nittany, the cause is unknown.
Treatment usually starts with medication. Even on medication, however, between 30% to 40% of Nittany's heartbeats were still abnormal. Given that Nittany was only a year old and would likely need lifelong therapy, Hsue saw an opportunity to leverage new technology and create a digital map of her heart to increase her odds of successful treatment.
"The use of electro-anatomical mapping was key to this whole process," Hsue says. "It's a technology that is relatively new to the veterinary field, and Cornell is one of the few places in the world that is pioneering it as a treatment for pets."
Hsue co-led the care team with adjunct professor Dr. Roberto Santilli and resident Robert Ciardullo, D.V.M. '21. Hsue received specialized training in utilizing new technologies for cardiac ablation prior to arriving at Cornell, while Santilli has 20-plus years of successful experience in performing cardiac ablation in dogs and is one of the few veterinarians in the world with this expertise.
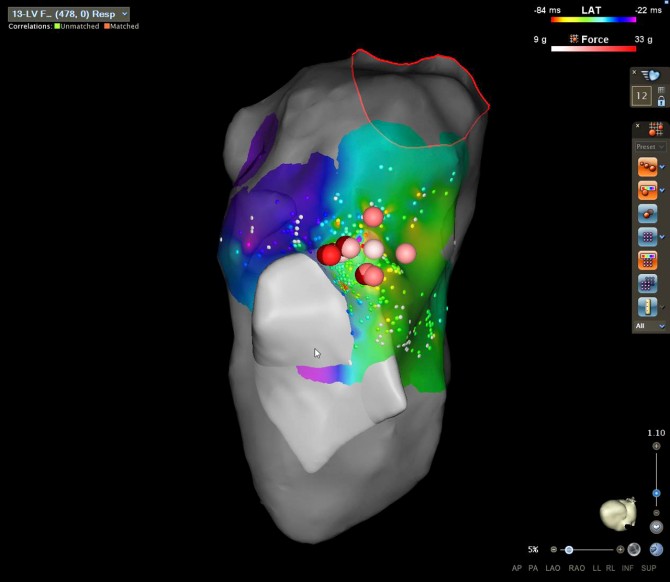
Electro-anatomical mapping allows veterinarians to create 3D reconstructions of a heart. A catheter that collects information on heartbeats is inserted in either the thigh or neck, is sent through a blood vessel into the heart, and tags the electrical information onto the 3D reconstruction. Nittany's ventricular arrhythmia was in a spot in the heart that was difficult for catheters to reach, so having a 3D map eased the challenges of the procedure.
"Unlike antiarrhythmic medications, we are addressing the disease at its source," Hsue says. From start to finish, it's a high-tech but minimally invasive procedure. "No open-chest surgeries needed," he says.
Added Santilli: "We used a combination of the standard technique - locating the problem area with an electrocardiogram - and translated that information into a 3D, color-coded map of Nittany's heart," he says. "Thanks to this new system, we're now getting the information much more easily that was so difficult to pinpoint before."
Having completed the map of Nittany's heart, the cardiology team could then take another catheter to target the cells at the root of the problem and destroy them with heat. Santilli's expertise and experience were instrumental in ensuring proper clinical use of the technology.
"After seven and a half hours, we got the call that the surgery was successful," Brandi Gwin says. "Drs. Ciardullo, Hsue and Santilli were wonderful. They took the time to sit and explain Nittany's diagnosis, the procedure and everything we should expect throughout the whole process."
Hsue attributes the surgical success to the wealth of experience among Nittany's care team, combined with a deep understanding of this new technology. "In addition to our cardiology team, the anesthesia and critical care services, with their exceptional dedication and skills, ensured that Nittany remained safe and stable despite her abnormal heart rhythm."
While Nittany will continue to have her heart evaluated periodically, for now she doesn't require active treatment.
Overnight, Nittany's heart began beating normally again. She was able to stop taking heart medication and return home the following day.
One month later, the team rechecked her heart rhythm over a 24-hour period. "We found that her ventricular arrhythmia disappeared," Hsue says. "That's terrific - and extremely uncommon for it to disappear entirely."
"Nittany is doing amazing," Brandi Gwin adds. "Her energy level has returned, and she is just as loving and goofy as ever."
While Nittany will continue to have her heart evaluated periodically, for now she doesn't require active treatment and can live a normal Great Dane life.
"Nittany had the best-case outcome," Hsue says. "The procedure eliminated both the arrhythmia and the need for lifelong medications."
At Cornell, the procedure costs are reduced for eligible families thanks to the Henry and Karen Silverman Initiative to Advance Treatment of Canine Arrhythmias. This initiative furthers the study, diagnosis and treatment of arrhythmias in dogs, and aims to educate pet owners and veterinarians about additional treatments for heart rhythm disorders.
"Nittany was beloved by all of us here because she had such a sweet demeanor," Hsue says. "We are glad she's back to her normal self."
This article is adapted from the original by Melanie Greaver Cordova, assistant director of communications at the College of Veterinary Medicine.
Nittany, a blue fawn Great Dane puppy, was suffering from a ventricular arrhythmia, a condition that causes the heart to beat abnormally. It's a common and often deadly condition in dogs, but the cure - cardiac ablation - is so specialized that few veterinary hospitals can do it. Cornell veterinarians and an innovative new 3D heart mapping technology enabled Nittany to fully recover.